Written by Steven Burns
From his column To Your Health
In family medicine practice, physicians deal with all kinds of illnesses. I get calls for respiratory infections, fevers, intestinal bugs, sprains, strains, depression, pain, cancer, fear of illness, chest pain, and so on. The list would take my entire column. Many illnesses I treat are minor and can be dealt with quickly, sometimes by advising that the problem is not dangerous, that I can see them next week, or by prescribing medication. But nothing gets my attention more quickly than saying, “I can’t move my arm.”
In some ways, it’s an easy call. I tell the person they may be having a stroke, to take an aspirin, and to dial 911—immediately. Slam-dunk. On the other hand, after we hang up, I have to make sure the person actually called 911 and arrived at the hospital, and then talk with the hospital doctor and family members, to make sure the patient gets the best care.
So, what is a stroke? It is a sudden loss of blood flow to an area of the brain. It is the fifth leading cause of disability in the United States. There are two major types: ischemic and hemorrhagic. An ischemic stroke is caused by a clot or piece of plaque that lodges in a blood vessel to the brain, blocking it, and resulting in sudden loss of blood flow to the area. Tissue damage starts immediately. This type accounts for 87% of strokes. A hemorrhagic stroke is caused by the rupture of a blood vessel. The blood then seeps into brain tissue and, again, the area served by the vessel does not get blood. Additionally, damage may be caused by the blood itself in the brain tissue.
Stroke associations add a third type of stroke, called a transient ischemic attack (TIA—sometimes called mini-strokes), although the designation is not completely accurate. By definition, a TIA resolves within 24 hours, while a stroke takes much longer. A TIA has no ongoing symptoms, hence the “transient” title. In this type of event, a blockage forms in an artery, and then clears, leaving behind no permanent brain damage.
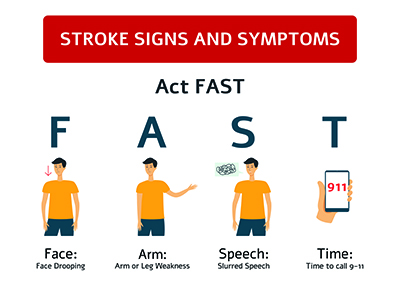
FAST Diagnosis
There is an acronym that can help with non-medical evaluation of neurological problems: FAST. The letters stand for Face, Arm, Speech, and Time, and everyone reading this article should memorize them—right now—because every minute counts when a person is having a stroke.
Facial drooping or asymmetry (one side appearing suddenly different from the other) can be an early sign of stroke, and may be associated with difficulty speaking caused by muscle paralysis of the mouth. Asking a person to smile can accentuate the abnormality.
Arm weakness or paralysis is sometimes not obvious, but if a person is asked to raise both arms and hold them together with their eyes closed, the weak one will typically drift downward.
Speech problems that occur with a stroke can be two-fold. One is dysarthria—difficulty moving the mouth to make the word. The other is aphasia—difficulty saying the right word, or sometimes any word at all. Ask the person to repeat a simple phrase. Does their speech sound slurred or strange?
Time refers to the necessity of getting the person help very quickly. This is one instance when you don’t wait an hour to see if it gets better. A patient has three hours from the onset of symptoms to get TPA (tissue plasminogen activator—a clot-dissolving chemical). Getting TPA can completely reverse the effects of a stroke, but it must be administered within three hours, measured from the last time the person was observed to be normal.
There are other signs of stroke, including sudden numbness, confusion, loss or blurring of vision, trouble walking, and severe headache. In the case of any of these symptoms, a visit to the emergency room is in order. By the way, when I talk about an emergency visit, I don't mean a drive to the hospital after getting all the things you might need if you have to stay overnight. I mean calling 911 and following the advice of the paramedics when they arrive.
The best treatment for stroke occurs in certified stroke centers. Hospitals with that designation follow specific protocols from the moment they get the call from paramedics and throughout the patient’s care. One guideline, for instance, is that patients will receive TPA (if appropriate) within 60 minutes of arrival at the emergency department. Try Googling “certified primary stroke center (name of your community)” today, and make note of the one you’d prefer (or covered by your insurance) in your phone contacts, so you’ll have it in an emergency.
I cannot stress enough the importance of knowing the symptoms of stroke, and having a plan to deal with them when they occur in yourself or others. As we grow older, each of us is at higher risk for stroke, because of other illnesses or just aging. Make sure you and those around you know what to do—then, act FAST!
Dr. Steven Burns is board-certified in family medicine and has been in practice for more than 30 years.